When you’re on treatment for osteoporosis, waiting a year or two to see if it’s working can feel like gambling with your bones. That’s where bone turnover markers come in - they give you real-time feedback, not a guess. Unlike bone density scans (DXA), which take 12 to 24 months to show meaningful changes, bone turnover markers can tell you within 3 to 6 weeks whether your treatment is having an effect. This isn’t theory - it’s clinical fact backed by research from the International Osteoporosis Foundation and Mayo Clinic Laboratories.
What Are Bone Turnover Markers?
Bone is never static. Every day, old bone breaks down (resorption) and new bone forms (formation). This process, called remodeling, is normal. But in osteoporosis, resorption outpaces formation, leaving bones weak. Bone turnover markers (BTMs) are tiny fragments and enzymes released into the blood or urine during this process. They’re like smoke signals from your bones - showing whether they’re breaking down too fast or building up properly.
There are two main types:
- Formation markers: These tell you how fast new bone is being made. The most reliable is procollagen type I N propeptide (PINP), also called P1NP. Others include osteocalcin and bone alkaline phosphatase.
- Resorption markers: These show how fast old bone is being broken down. The gold standard is β-isomerized C-terminal telopeptide of type I collagen (β-CTX-I), often just called CTX. Urinary NTx and TRACP5b are also used.
According to the 2023 consensus from the International Osteoporosis Foundation and European Calcified Tissue Society, PINP and β-CTX-I are the only two markers recommended for routine clinical use. Why? Because they’re the most stable, accurate, and least affected by things like meals or time of day.
Why Use Them Instead of Just a DXA Scan?
DXA scans measure bone mineral density - how thick or dense your bones are. That’s important, but it’s slow. If you start a new osteoporosis drug, you won’t see a meaningful change on your DXA for at least a year. By then, you might have already broken a bone.
Bone turnover markers change much faster. For example:
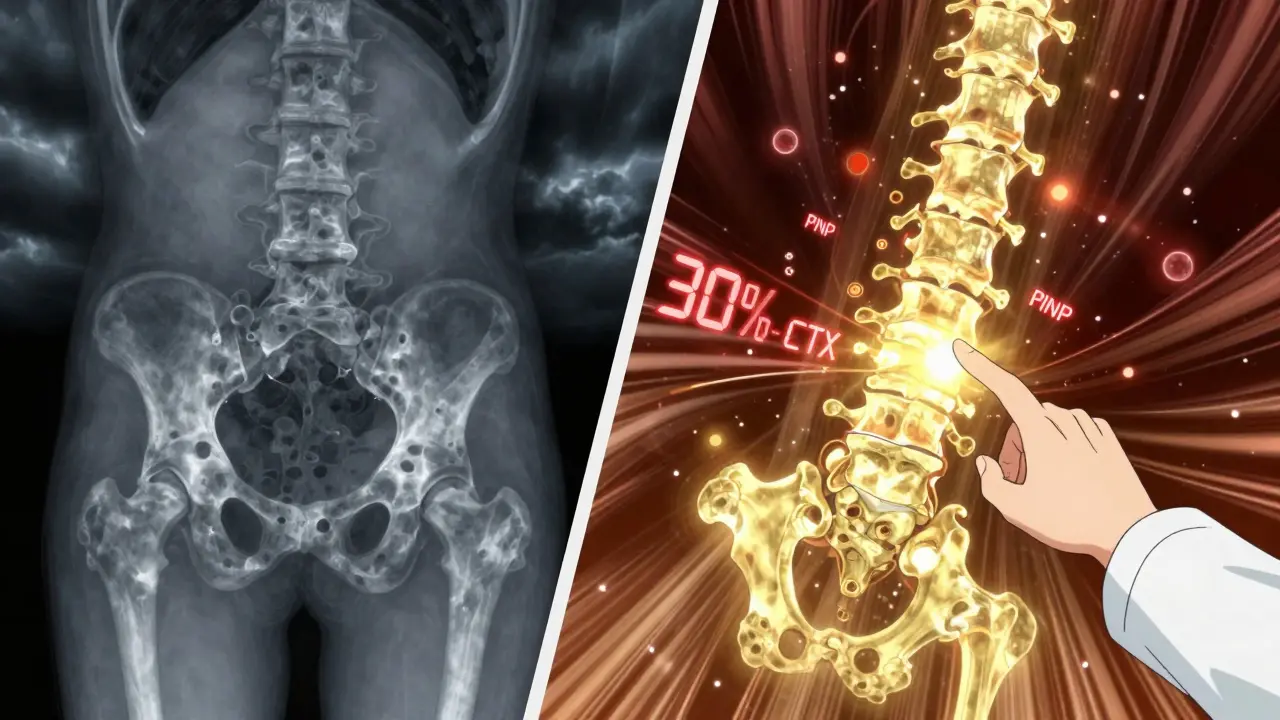
- If you’re on a bisphosphonate (like alendronate or zoledronic acid), your CTX levels should drop by more than 30% within 3 to 6 months. That’s a sign the drug is working.
- If you’re on an anabolic drug like teriparatide, PINP should spike by 70-100% within 1 to 3 months - showing your body is building new bone.
The TRIO study found that patients who hit a 30% drop in CTX at 3 months had a 1.6% lower fracture risk after just 22 weeks. That’s a direct link between early marker changes and real-world outcomes.
Think of it this way: DXA is like checking your car’s odometer to see how far you’ve driven. BTMs are like checking the engine light - they tell you if the system is running right right now.
How Are They Measured? What Do You Need to Know?
Getting accurate results isn’t as simple as walking into a lab. These markers are sensitive to timing, food, and even your body’s natural rhythms.
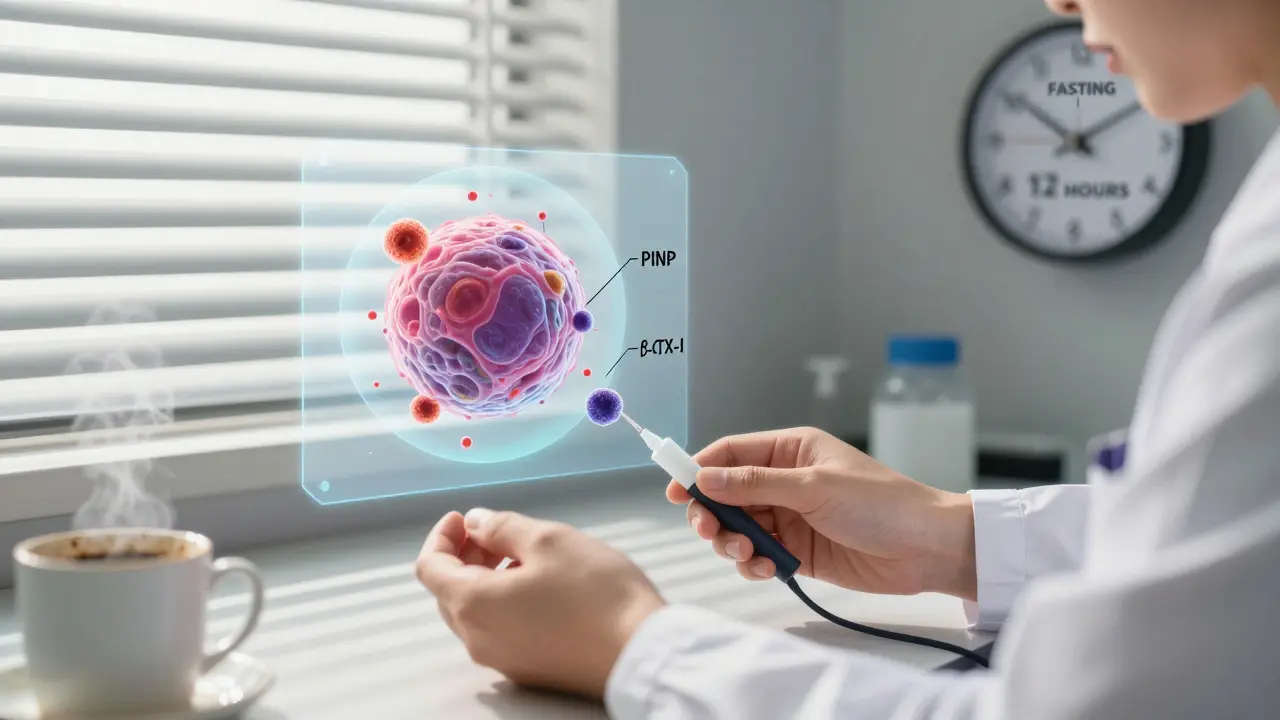
For β-CTX:
- Must be drawn in the morning, between 8 and 10 a.m.
- You need to fast overnight - no food, coffee, or even water before the test.
- Post-meal levels can jump 20-30%, throwing off results.
- Diurnal variation (natural daily changes) can swing CTX levels by up to 40% if not timed right.
For PINP:
- Less affected by meals - but still best to test in the morning.
- Diurnal variation is smaller (10-15%), making it slightly easier to manage.
Lab precision matters too. The best assays for PINP have an intra-assay coefficient of variation (CV) of just 5.8%, and for β-CTX, it’s 3.5%. That means if you test the same sample twice, you’ll get nearly the same result. But not all labs are equal. Only about 65% of U.S. labs follow the IFCC-recommended protocols. Always ask if your lab uses standardized methods.
What’s a Meaningful Change?
Not every number change means something. The body has natural noise. That’s why experts use something called the least significant change (LSC).
- For PINP: A change of 20% or more is considered real.
- For β-CTX: A change of 25% or more is meaningful.
So if your baseline CTX is 0.5 ng/mL and it drops to 0.4 ng/mL (a 20% drop), that’s not enough. But if it drops to 0.35 ng/mL (a 30% drop), that’s a strong signal your treatment is working.
For anabolic drugs:
- A 70-100% rise in PINP within 3 months is considered a good response.
- Anything less than 35% increase might suggest poor response or non-adherence.
Who Benefits Most From BTMs?
Not everyone needs them. But here’s who does:
- Newly diagnosed patients: Starting treatment? Test BTMs before you begin, then again at 3 months. This sets a baseline and catches early problems.
- Non-adherent patients: If you’re not taking your meds, your BTMs won’t move. Studies show BTMs can identify non-adherence with 85% sensitivity. That’s more accurate than asking.
- Patients on high-risk therapies: Those on long-term bisphosphonates or anabolic agents need to know if the treatment is still working - or if side effects are outweighing benefits.
- Patients with kidney disease: Standard markers like PINP and CTX can be falsely elevated due to reduced clearance. In CKD, bone alkaline phosphatase (BALP) and TRACP5b are better alternatives.
For everyone else - routine BTM testing isn’t needed. Your DXA scan every 1-2 years is still the gold standard for long-term tracking.
Limitations and Pitfalls
Bone turnover markers aren’t perfect. Here’s what you need to watch out for:
- Not site-specific: They tell you what’s happening overall in your skeleton, not in your spine or hip. That’s why DXA still rules for fracture risk prediction.
- Biological variability: Stress, illness, or even a bad night’s sleep can affect levels. That’s why repeat testing at the same time of day, fasting, and under the same conditions is critical.
- Reference ranges aren’t universal: Most reference values come from Caucasian populations. Asian populations often have 15-20% lower baseline CTX. African populations show 10-15% higher PINP. Labs need to adjust for ethnicity - but many don’t yet.
- Cost and access: Medicare covers PINP (CPT 83970) and CTX (CPT 83935), with reimbursement around $30 per test. But not all insurers do. In Europe, 45-60% of clinics use BTMs. In the U.S., it’s still only 25-35%.
What’s Next? The Future of BTMs
The field is moving fast. The American Association of Clinical Endocrinologists plans to update its guidelines in Q2 2024 to include specific BTM recommendations. Point-of-care tests - where you get results in minutes at your doctor’s office - are in development. If they get FDA clearance and CLIA-waived status, BTMs could become as routine as a cholesterol test.
Research is also expanding into how BTMs predict fracture risk beyond just monitoring treatment. Trials like NCT04567821 are testing whether adjusting drug doses based on BTM levels leads to fewer fractures than standard care.
And the big picture? Experts agree: bone turnover markers aren’t replacing DXA. They’re completing it. A full osteoporosis management plan should include:
- Baseline DXA scan
- Baseline BTM test (PINP and β-CTX-I)
- Repeat BTM at 3 months
- DXA repeat at 12-24 months
If your BTMs move the right way at 3 months, you’re on track. If they don’t, you can switch drugs, fix adherence, or adjust your dose - before it’s too late.
Bottom Line
Bone turnover markers are not a luxury. They’re a tool that turns guesswork into action. If you’re on osteoporosis treatment, ask your doctor: “Have you checked my bone turnover markers?” If they haven’t, it’s not because they’re not useful - it’s because they’re still underused. With the right timing, the right lab, and the right interpretation, these tiny markers can save you from fractures, unnecessary drugs, and years of uncertainty.


Hi, I'm Caden Lockhart, a pharmaceutical expert with years of experience in the industry. My passion lies in researching and developing new medications, as well as educating others about their proper use and potential side effects. I enjoy writing articles on various diseases, health supplements, and the latest treatment options available. In my free time, I love going on hikes, perusing scientific journals, and capturing the world through my lens. Through my work, I strive to make a positive impact on patients' lives and contribute to the advancement of medical science.